Understanding rotator cuff tears
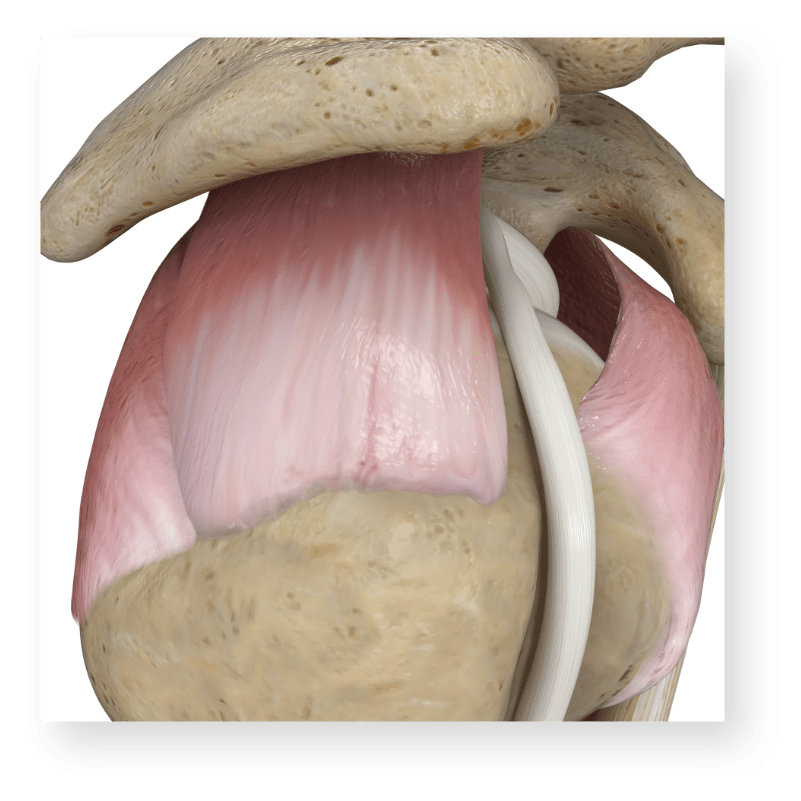
Healthy rotator cuff
Rotator cuff tear types
When your doctor tells you that you have a rotator cuff tear (RCT), it is because one or more of the four muscles that make up the cuff is injured. RCTs are amongst the most common joint injuries in adults. Tears of your rotator cuff are a common source of pain, weakness, and loss of function of your shoulder affecting the ability to perform even the easiest activities of daily living. Rotator cuff tears can be due to the natural worsening of the rotator cuff over time or can be from an injury. These tears will vary in severity and include the following types:
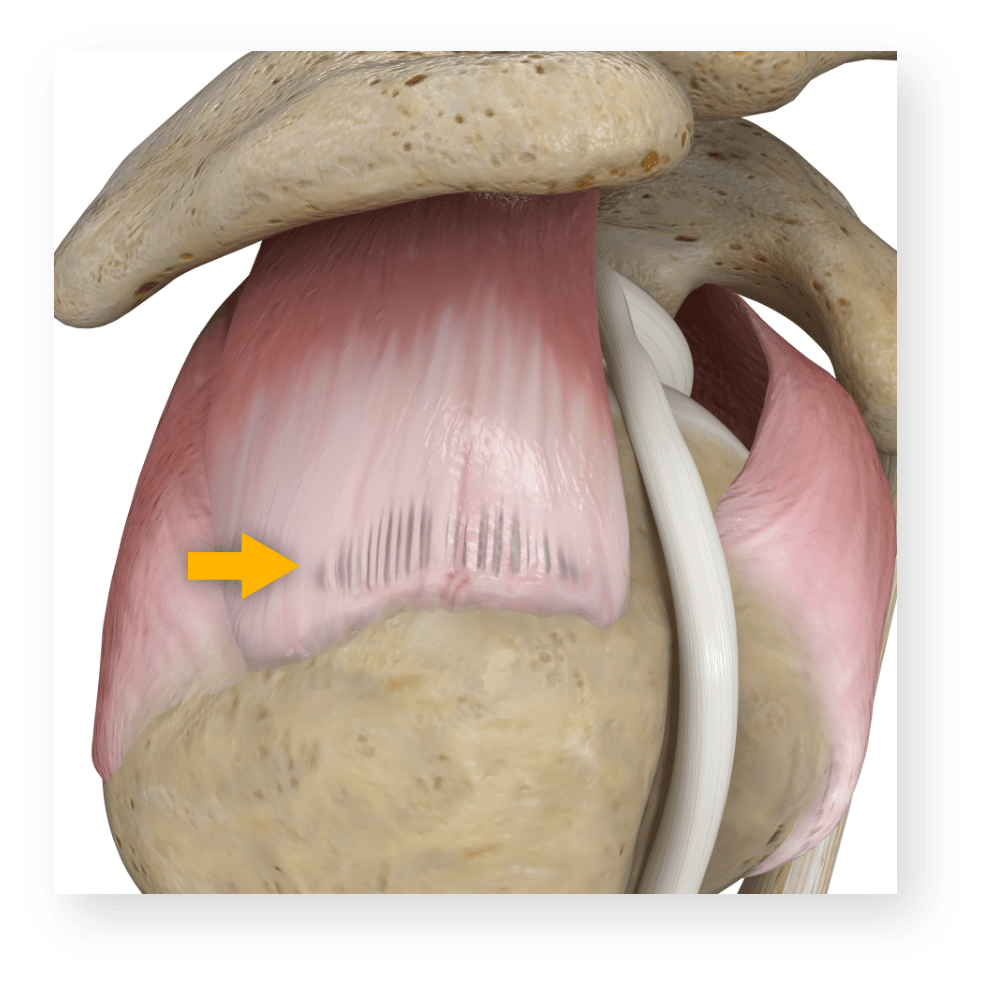
Partial Thickness RCTs
Tears that are incomplete or do not involve the full thickness of a muscle or tendon of your shoulder.
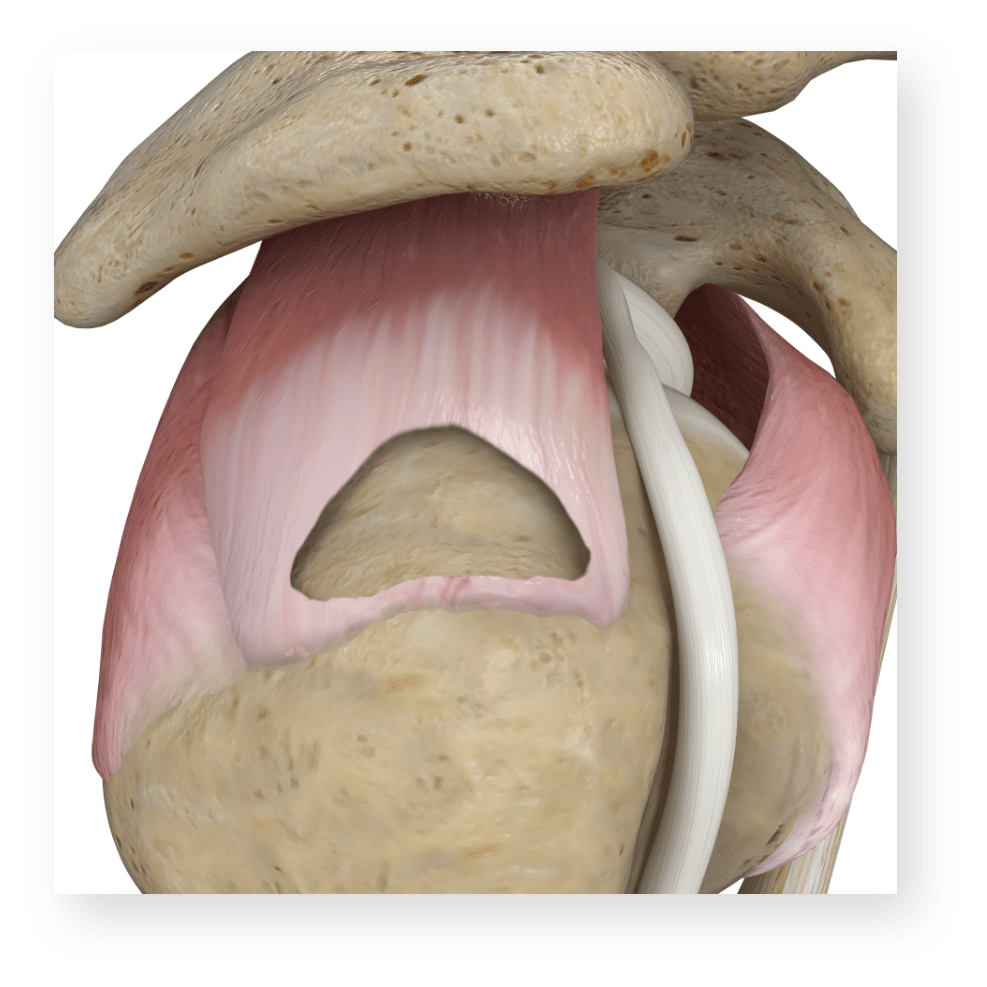
Full Thickness RCTs
Physical therapists can help lessen your pain by teaching better posture or "form" for your day-to-day activities, like getting in Tears that involve the entire thickness of a muscle or tendon of your shoulder.
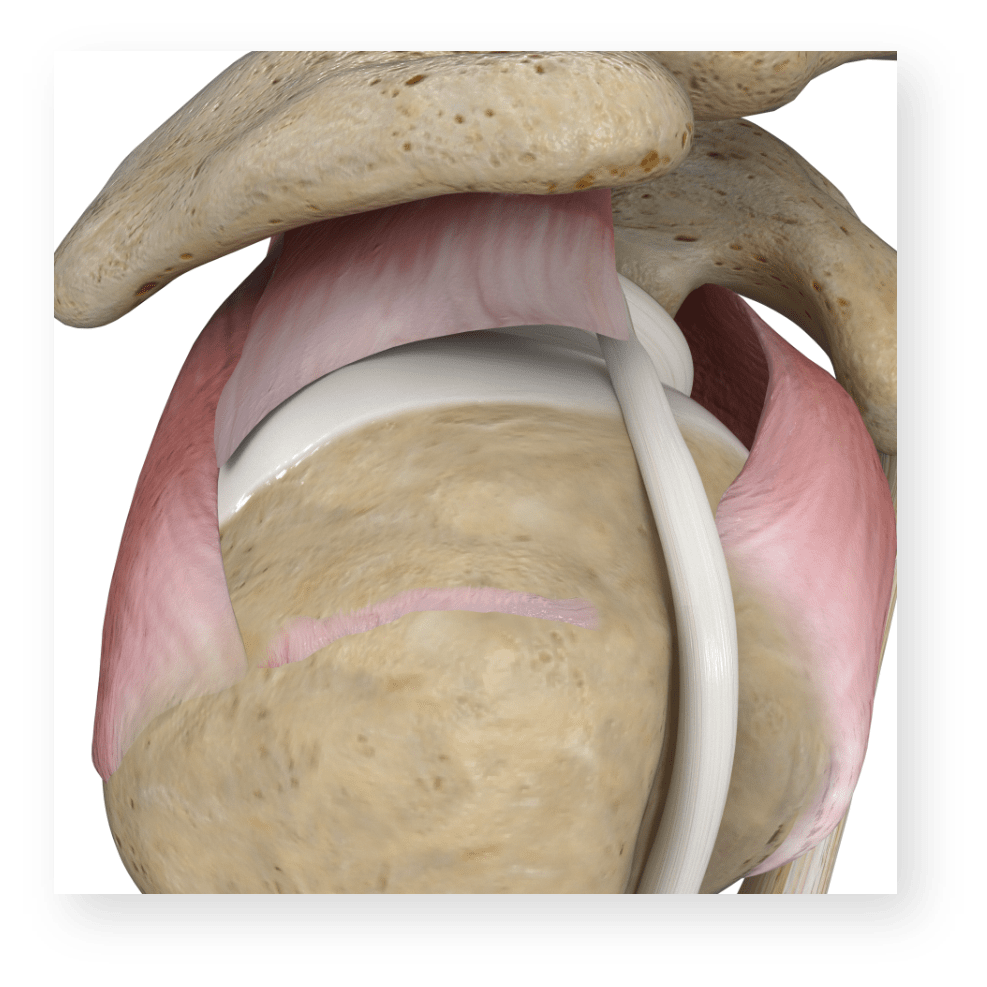
Massive RCTs (MRCTs)
Described as the rupture of at least two of the four rotator cuff tendons and/or pulling away from the place where the tendons attach in your shoulder of 5 cm (which is approximately 2 inches) or greater. MRCTs may be reparable or not. If they are not reparable, then are referred to as Massive Irreparable RCTs (MIRCTs).
Talk to your doctor
While every doctor is different, many will follow a similar approach to helping you understand your shoulder pain. At your first appointment, your doctor may ask you a few questions about when and where your shoulder hurts to assess what’s going on. The doctor may also ask you to have additional diagnostic tests, like an X-ray, ultrasound or MRI. These imaging tests are usually required to confirm whether or not you have a rotator cuff tear (RCT).
It is important to understand that when it comes to rotator cuff injuries, there are multiple treatment options, and pain relief does not always mean surgery. Learn more about your options below.
Treatment options
The best treatment is the one that works for you. Doctors may start by recommending treatment to reduce the swelling, quiet the pain and get you moving without surgery. But sometimes that’s just not enough. Your doctor can help guide you through your treatment choices.

Treatment without surgery
Lifestyle changes, physical therapy, rest, ice, over-the-counter anti-inflammatory, pain medicines or steroid injections may help reduce the swelling and pain in your shoulder joint.
LEARN MORE
Shoulder arthroscopy surgery
Shoulder arthroscopy is a type of surgical procedure that uses a tiny camera called an arthroscope to examine and prepare the tissue inside and around your shoulder joint. The arthroscope is inserted through a small cut in your skin and allows your surgeon to better visualize the condition of your shoulder joint so they can determine an appropriate solution.
While all shoulder arthroscopy surgery does have risks, one of the benefits to this approach is that this surgery is typically done on an outpatient basis, so you will likely return home the same day.
LEARN MOREIMPORTANT INFORMATION ABOUT INSPACE
The InSpace Implant is indicated for the treatment of patients with massive, irreparable full-thickness torn rotator cuff tendons due to trauma or degradation with mild to moderate gleno-humeral osteoarthritis in patients greater than or equal to 65 years of age whose clinical conditions would benefit from treatment with a shorter surgical time compared to partial rotator cuff repair.
The InSpace Implant is not appropriate for patients with certain types of infections, known or suspected allegories to the implant and/or instrument materials, or children.
The following information provided is based on data collected in the US Pivotal Clinical Study. There is evidence of increased risk of total adverse events of the affected shoulder compared to a partial rotator cuff repair, which were reported to be mostly mild to moderate in severity. Please note that complications reported by InSpace and Partial Repair patients were reviewed by a group of experts in shoulder surgery, and it was determined that none were related to the treatment devices (i.e., the InSpace Implant or devices used for Partial Repair). There is evidence of increased adverse events associated with a serious risk of the index shoulder which includes both medical and surgical treatments. The InSpace Implant is not fixed in place and may change position in the shoulder space. Movement out of the subacromial space and/or deflation of the InSpace Implant was observed in magnetic resonance imaging (MRI) 6 weeks post-operatively in up to half of patients. In these cases, it should be noted that no re-operations were required to remove the InSpace Implant.
The risks and benefits of the InSpace Implant in patients with the following conditions should be carefully considered: severe arthritis in the shoulder or full thickness cartilage loss, deltoid muscle defect or deltoid muscle paralysis, evidence that the shoulder is very unstable, missing or non-intact ligaments in the shoulder, known loss of sensation, major medical conditions such as blood clotting disorders, conditions that suppress the immune system or any other conditions that may compromise healing, safety and effectiveness of InSpace Implant use in patients below age sixty-five (65) has not been established, and safety and effectiveness of InSpace Implant use in pregnant or nursing mothers has not been evaluated.
If a reaction occurs, it will require follow-up with your surgeon. Some examples are as follows: irritation at the site where a cut was made during surgery, local infection, inflammation, and tissue damage where the InSpace Implant was implanted, or worsening of an existing infection. Additionally, movement of the implant out of its intended location may lead to worsening of your shoulder pain, discomfort, and/or stiffness which may require a re-operation, narcotic medications, non-narcotic pain medications, or post-operative shoulder injections.
As with any surgery, your surgical procedure may cause complications or adverse events. As with any shoulder surgery involving anesthesia there are potential risks and complications, including dizziness, fainting, difficulty breathing, wound infection, wound drainage, swelling, local pain, bleeding, bruising, surgical wound opening, nerve pain or injury which could result in partial or complete loss of movement in your affected arm, tendon injury, loss of sensation in your skin and muscle around your surgical site, inflammation of the tissues that surround your rotator cuff joint, a frozen rotator cuff (inability to freely move the shoulder joint) and delayed wound healing. There is a risk that a deep vein clot will form (thrombosis) and travel to the lung (pulmonary embolism), which could lead to stroke, heart damage or death. Any of the aforementioned complications/risks could require treatment such as medicine or additional surgery that may involve replacing or removing your InSpace Implant dependent on timeframe as the implant is biodegradable.
The information presented is for educational purposes only. Speak to your doctor to decide if you are interested in learning more about the InSpace Implant. Individual results vary and not all patients will receive the same postoperative activity level. It is important to follow your surgeon’s advice regarding after surgery care (for example, physical therapy) as well as which immediate activities you may or may not perform after receiving the InSpace Implant. Not following this advice may cause complications with the InSpace Implant. Some complications may require you to have additional surgery. Ask your doctor if the InSpace Implant is right for you.
Stryker Corporation or its other divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: InSpace, Stryker, Together with our customers, we are driven to make healthcare better. All other trademarks are trademarks of their respective owners or holders.
1000904124 Rev A